Years of Experience
Surgeries Performed
Patient Reviews
Years Pro Baseball MD
Athletic Teams
Education & Medical Training
Extensive academic and clinical foundation in Orthopaedic Surgery and Sports Medicine
Dr. Galland earned his medical degree and completed his residency in Orthopaedic Surgery at Tulane University School of Medicine, where he trained under renowned sports medicine specialist Dr. Michael Brunet. He holds board certifications in both Orthopaedic Surgery and the subspecialty of Orthopaedic Sports Medicine.
Medical School
Tulane University School of Medicine
Board Certification
American Board of Orthopaedic Surgery (2001)
Residency
Tulane University Department of Orthopaedic Surgery
Subspecialty Certification
Dr. Galland's Practice
Specialized Treatment for Athletes and Active Patients
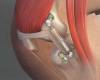
ACL Reconstruction
Shoulder Arthroscopy
Sports Injury Care
Knee & Joint Preservation
Elbow & Throwing Injuries
Athlete Performance Medicine

Start Your Free Imaging Review Today
Free X-Ray & Imaging Review
Upload your existing x-rays or imaging, and Dr. Galland will personally review them to help you understand your treatment options.
CARE THAT MAKES A DIFFERENCE.
“Dr. Galland was exceptionally personable, relatable, and thorough. He took the time to fully understand my concerns rather than rushing through the appointment. I genuinely appreciate his thoughtful approach and the care he showed in treating me as a patient.”

Team Physician
Specialized Treatment for Athletes and Active Patients


















Patient Testimonials
Compassion, trust, and exceptional care.
Don’t take our word for it – hear from patients who’ve worked with Dr. Galland.
Get in touch
We’d love to hear from you! Whether you’re a new or returning patient, have a question about our services, or would like to schedule an appointment, our team is here to help.
OrthoNC
11221 Galleria Ave, Suite 101, Raleigh, NC 27614
info@drgalland.com